In addition to the immediate risk of coronavirus pandemic, there is the longer-term concern as to the continued role that coronavirus will play in our society. Complete elimination of the novel coronavirus from the human population is exceedingly unlikely, not to mention the added risk of reintroduction from an animal reservoir in the future assuming we do somehow manage it.
This all suggests that businesses will need to continue to take serious precautions in the immediate future to protect their employees, their customers, and their finances, especially in light of questionable and fractured government action*. However, there are many other reasons to take the risk management lessons learned from this epidemic seriously, and to extend at least some of them beyond the year or two that it will hopefully take for the situation to resolve.
One common fear is the risk of this coronavirus mutating into something that makes the illness more severe, or else that bypasses immunity that had been developed through sickness or vaccination. It is true that coronavirus mutates rapidly, and new research suggests that there are many more strains of the virus than previously thought, including some that might be much more virulent than others. However, this difference was found in samples taken near the beginning of the epidemic, meaning that they’ve been with us since then. Generally, it’s unclear whether the disease would be capable of a mutation that would make it much more deadly than it already is, though it is unlikely. Indeed, viruses often mutate into less deadly versions of themselves over time due to selection pressure. As far as immunity, the mechanism that the flu undergoes that makes immunity to it so temporary is not something that coronavirus can do; there are many vaccines for viruses with a rate of mutation similar to coronavirus, like measles, that have continued to work after decades. That being said, it is still too early to know anything for sure, and there is a body of research that suggests that this could still be a concern.
Even without mutation, the nature of coronavirus immunity is still unclear – for example, while reinfection is unlikely, we don’t have a very good idea of how long immunity lasts. As immunity develops or a vaccine is introduced, it is likely that the disease will at the very least become less fatal; whether or not this coronavirus becomes a seasonal illness, like the flu, or endemic, like many other coronaviruses that cause the common cold, is still unclear, but these do seem to be the two most likely options.
However, the possibility that coronavirus could become a seasonable disease raises some interesting points. Anecdotal evidence suggests that social distancing has significantly reduced the transmission of the flu, a disease which regularly kills far more people in the United States than have died from coronavirus so far. The spread of other diseases has almost certainly dropped as well (not to mention the number of car accidents). In that sense, reinforcing at least some of the behaviors and policies that we are currently practicing due to coronavirus is likely to decrease the number of people who die under non-pandemic circumstances.
It’s also worth talking about the potential for other pandemics. This coronavirus pandemic was neither unexpected nor unprecedented. Just in the past two decades, we have seen two other coronavirus outbreaks – SARS and MERS – that were successfully contained.
It is likely that there is something different about this coronavirus that made containment more difficult – possibly the fact that individuals are infectious before showing symptoms. After all, while China has been criticized for its handling of the current coronavirus, similar issues with the Chinese response occurred during the SARS outbreak.
That isn’t to say that it would not have been possible to eliminate COVID-19 in the same way that SARS was eliminated, assuming other circumstances. However, even governments that are widely recognized as having responded appropriately since the beginning, like Taiwan, have been unable to completely eliminate the disease within their borders.
Regardless of how unusual this coronavirus is, though, it would be arrogant to presume that there is no likelihood of another global pandemic in the future. Epidemiologists had been warning of this possibility for years – in fact, coronaviruses are one of a handful of viruses that had long been identified as potential sources of a global pandemic. It is true that significant changes to animal supply chains are needed, especially in the case of the more egregious wet markets that seemed to have provided the conditions for this pandemic to take place (and if your business involves the handling of animals, then the risk of zoonosis is without question something that you should take seriously, if you haven’t already). However, these precautions will not eliminate the risk, they will merely reduce it.
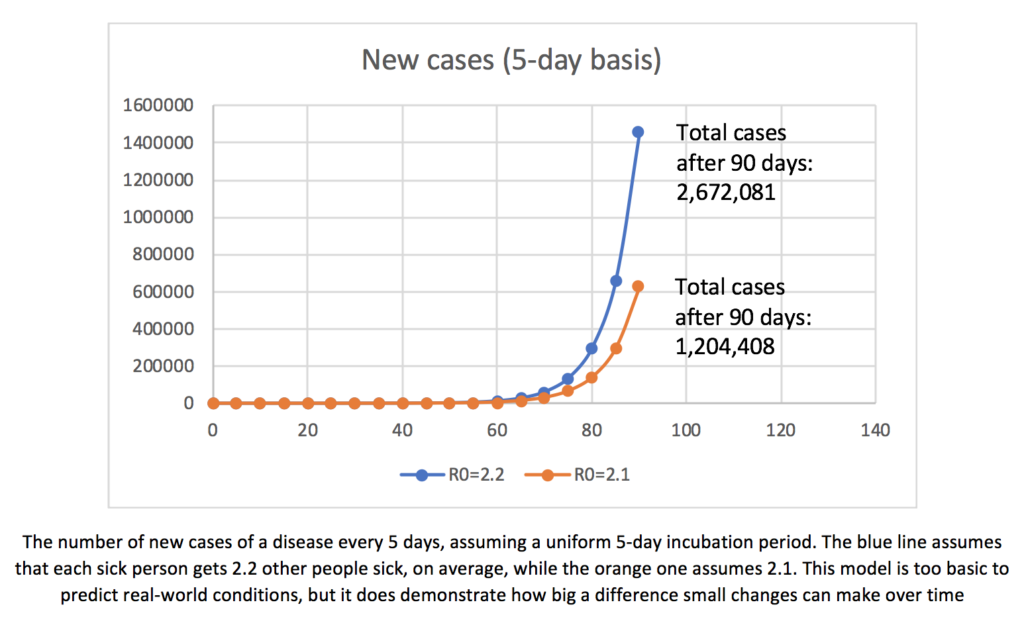
If broader hygiene measures, like handwashing**, were not already practiced on a broad level in our society, coronavirus would have spread far more quickly. However, if there were other practices established in our homes and businesses that were as standard as handwashing is (presuming of course that handwashing is standard, which, if it isn’t, would be a great place to start), coronavirus would have spread more slowly. This would have saved lives and given our government more time to prepare a less destructive and more effective response. Such measures might still save many lives (and money) going forward during this pandemic. And while these measures might not stop an epidemic in the future (although they certainly could help), the nature of exponential disease growth means that making even small changes in our behavior and society could have big returns going forward.
Taking these measures wouldn’t simply be altruistic; they would have serious benefits for businesses, as employees would get sick less – under all circumstances – and productivity would be less affected. There are plenty of things that you, as a business owner, can do to create a work environment that is more resilient to disease. We’ve already discussed some of these ideas in earlier posts, but we’ll be sure to go into more detail in another one, coming soon.
*Many states have begun to ease restrictions, prompting concerns of another peak. For one thing, the total number of confirmed US cases has increased from about 650,000 to roughly 1,000,000, even while it has slowed dramatically in certain places, especially New York City. In fairness, this increase in case number is likely due to a significant backlog in testing more than anything else, and there is already plenty of evidence that lockdowns and social distancing have had a measurable effect on the spread of coronavirus across the country. However, the lack of sufficient testing in itself means we have no way of knowing how damaging reopening might be.
That being said, we are now starting to get an idea of how many people have been infected. New York State recently announced results from antibody testing, which suggest that as many as 21% of the residents of New York City have already been infected with the virus. This is good news, but only conditionally.
On the one hand, when combined with the total number of deaths in the state, it suggests that the mortality is somewhat lower than previously feared, at about 0.5%. However, there are questions as to the accuracy of antibody testing. The testing protocol may have also led to overcounting, while the total number of deaths is likely much higher than the official count. Worst of all, 21% is still well below even the most hopeful estimates of what is needed for herd immunity, as we discussed previously. Considering that New York City was hit harder than anywhere else, this further suggests that herd immunity is not an achievable goal in the near future – after all, New York antibody rates outside of the New York City metro area were measured at only 3.6%, while additional research in Santa Clara County in California showed potential rates between 2.5% and 4.2%.
**As part of doing research into this article, we read a bit about Mary Mallon, also known as Typhoid Mary. Mary worked as a cook in New York City in the early 1900s, and in doing so, infected many of her clients with typhoid; she was a carrier of the disease her entire life, but never got sick from it. What might be most interesting about her case is that she apparently never washed her hands – this wasn’t as common a practice in her time as it is today. While it’s very likely that Mary would still have infected many people with typhoid, there’s no question that the death toll would have been far lower had she taken this simple preventive measure.
It is interesting to consider how certain other practices – like widespread use of masks, or flexibility with working from home – might be seen in the future in the same way that we look at handwashing today.

